By – James M. Katz, BA
In recent years, the search for effective mental health therapies has led to a renewed interest in the benefits of eft training (Emotional Freedom Techniques). This innovative approach, combining elements of cognitive behavioral therapy and traditional Chinese acupressure, targets the mind-body connection to alleviate psychological stress and emotional distress. EFT tapping, or emotional freedom tapping, offers a compelling alternative to conventional treatments, promising relief from anxiety, depression, and other emotional disorders. Its significance lies not only in its effectiveness but also in its accessibility, providing tools that individuals can use practically anywhere, making it a pivotal development in the landscape of mental health therapy.
This article delves into the multifaceted advantages of EFT, exploring how eft techniques and tapping therapy can profoundly impact emotional well-being. It highlights the importance of understanding the mind-body connection, the role of EFT in handling trauma, and its benefits for non-verbal individuals—underscoring the critical importance of proper training for practitioners. Additionally, it discusses moving beyond medical models, explaining EFT tapping sessions, and integrating EFT with other modalities like cognitive behavioral therapy, further expanding its utility and effectiveness. Through this exploration, readers will gain a comprehensive understanding of what is eft tapping and the broad spectrum of eft benefits, showcasing why tapping for anxiety and other emotional challenges holds a promising place in the future of mental health therapy.
Key Takeaways
- EFT training enhances emotional intelligence and self-regulation, leading to improved client outcomes.
- Certified EFT practitioners enjoy increased earning potential and expanded career opportunities.
- EFT training provides advanced techniques for managing stress, anxiety, and emotional trauma.
- Professionals trained in EFT can build stronger personal relationships through better communication and conflict resolution skills.
- Continuous professional development opportunities in EFT ensure practitioners stay updated with the latest research and practices.
- Understanding Emotionally Focused Therapy (EFT)
- Emotionally Focused Therapy (EFT) is a humanistic, evidence-based approach to psychotherapy that emphasizes the central role of emotions in human experience.
Developed by Dr. Sue Johnson in the 1980s, EFT is grounded in Attachment Theory and Emotion Regulation Theory. EFT helps clients identify and transform negative processing and interaction patterns that create distress. It’s effective in treating individuals, couples, and families, addressing a wide range of issues from marital conflicts to emotional trauma.
Understanding EFT Tapping
Emotional Freedom Technique (EFT) tapping, often referred to as psychological acupressure, is a method that combines elements of cognitive behavioral therapy and acupressure to address emotional distress and physical pain. Unlike traditional acupuncture, which uses needles, EFT employs fingertip tapping to apply pressure on specific meridian points of the body.
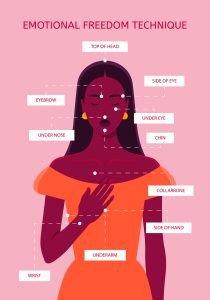
The technique is based on the premise that emotional issues are caused by disruptions in the body’s energy system. By tapping on these meridian points—areas where energy is believed to flow—individuals can restore balance and alleviate stress, anxiety, and other negative emotions. EFT tapping is designed to target the 12 specific meridian points on the body that correspond to different emotional states. Each point is tapped while the individual focuses on a particular negative memory or issue, effectively addressing the emotional impact of the problem.
This method has been adopted widely due to its simplicity and the fact that it can be practiced independently or with the guidance of a practitioner. During a session, individuals typically begin by identifying the issue and rating their level of distress. They then articulate a ‘set-up’ statement that acknowledges the problem while affirming self-acceptance. As they tap each meridian point, they repeat a reminder phrase to maintain focus on their issue.
EFT has gained popularity not only for its effectiveness in treating a range of issues like anxiety, depression, and PTSD but also because it provides a tool for individuals to actively contribute to their own healing process. The tapping technique is easy to learn and can be used as a self-help tool, making it accessible to a wide audience.
By integrating EFT with other therapeutic modalities, practitioners can offer a holistic approach to emotional wellness, emphasizing the importance of both mind and body in achieving emotional balance and health.
Mind-Body Connection
The concept of the mind-body connection underscores the profound interplay between our physical and emotional well-being. This relationship is evident as the body often signals its need for attention through various symptoms, such as shifts in energy or emotional changes. Emotional Freedom Technique (EFT) tapping, a method that merges cognitive behavioral therapy with acupressure, leverages this connection by targeting the body’s energy meridians. These meridians, akin to highways within the body, can be stimulated through tapping to foster both emotional and physical healing.
Research supports the effectiveness of EFT in addressing not only emotional distress but also physical symptoms. By tapping on specific meridian points while focusing on emotional issues, individuals can release energetic blocks, leading to improved well-being across physical, emotional, and spiritual dimensions. This holistic approach is further validated by neuroimaging studies, which show that EFT can modulate brain activity in areas related to emotion regulation and stress response, thereby enhancing emotional resilience and reducing stress.
The mind-body connection is not just a theory but a practical reality that can be harnessed for healing. For instance, chronic stress often manifests physically as ailments like back pain or digestive issues, which are in fact expressions of emotional turmoil. Addressing these emotional underpinnings through techniques like EFT can lead to significant improvements in both mental and physical health.
In summary, understanding and utilizing the mind-body connection through practices such as EFT can lead to a more integrated approach to health, where emotional and physical healing occur in tandem. This holistic perspective not only enhances individual well-being but also may shift how we approach health care, emphasizing the interconnectedness of our emotional and physical states.
Handling Trauma
Trauma profoundly impacts cognitive schemas, often undermining beliefs about oneself and altering perceptions of reality, which can disrupt daily life significantly without an individual’s awareness. Emotional Freedom Techniques (EFT) have been recognized for their extensive effectiveness in addressing trauma. They provide immediate relief and are gentle tools for uncovering and systematically working through the complex layers associated with trauma until their emotional charge dissipates.
For therapists, self-examination is crucial before engaging with clients’ trauma. It’s essential to resolve any personal unresolved trauma to avoid being triggered by clients’ experiences. This distinction between empathizing and colluding with clients is vital for effective therapy, ensuring therapists remain clear channels to serve their clients optimally.
Trauma is categorized into four broad types: prolonged past traumatic experiences, ongoing trauma, one-off trauma, and perceived trauma. Each category requires tailored approaches during EFT sessions. For some clients, immediately discussing their traumatic experiences is necessary, which can cause significant disruptions in their energy systems requiring continuous tapping. Others might present physical symptoms like insomnia or migraines, with no apparent connection to traumatic events. Here, therapists’ detective skills are crucial to gently uncover any related traumatic events.
For clients detached from their trauma, exhibiting symptoms like depression or anxiety, therapists must employ strategies to elicit specific emotional contributors underlying these symptoms. Post-Traumatic Stress Disorder (PTSD), whether from a single event or prolonged exposure, stores traumatic memories as if they are current, leading to flashbacks, hyper-vigilance, and other severe symptoms. These individuals might withdraw from life, viewing the world as unsafe, which necessitates a careful, gradual therapeutic approach.
EFT offers various techniques for handling trauma, including the Tearless Trauma Technique, Movie Technique, Telling the Story, Tsunami Technique, and Imagination Technique. These methods help clients dissociate from intense emotions safely and gradually, making EFT a versatile tool for trauma therapy. The effectiveness of EFT in trauma therapy is further supported by its ability to produce results in fewer sessions compared to traditional methods, with minimal risk of re-traumatization, and outcomes confirmed by biological, neurological, and genetic measures. Additionally, EFT equips individuals with effective coping strategies for future challenges, enhancing long-term emotional resilience.
Benefits for Non-Verbal Individuals
Emotional Freedom Techniques (EFT) tapping provides unique advantages for non-verbal individuals, particularly those within the autism spectrum who may experience challenges in traditional therapeutic settings due to difficulties in verbal communication. The tactile nature of EFT tapping offers a sensory-based method to aid in self-regulation and emotional management.
Children with Autism often require sensory stimulation to manage emotions and self-regulate. Tapping serves as a safe alternative to self-soothing behaviors that might be disruptive or unsafe. This method involves tapping on specific meridian points on the body, which can mimic the soothing effects of stimming behaviors, providing a repetitive, calming sensation.
The application of EFT tapping with non-verbal individuals must consider their cognitive abilities and the extent of their communication challenges. While there is a lack of specific research focused solely on non-verbal groups, studies on the efficacy of tapping for those with anxiety disorders suggest that EFT can be beneficial for those needing relief from emotional distress. The technique’s simplicity allows for easy adaptation to various needs, including those who are non-verbal, making it a versatile tool in emotional therapy.
Furthermore, the movements involved in tapping not only offer a physical outlet for emotional expression but also help in reducing stress and anxiety, common issues faced by individuals on the autism spectrum. It is crucial, however, to tailor the approach to each individual’s cognitive development and ability to engage with the technique, ensuring they can effectively learn and apply the tapping methods to manage their emotions independently.
In cases where individuals are diagnosed with more profound verbal and non-verbal deficits, such as ASD Level 3, the effectiveness of EFT may vary, and adaptations to the standard protocol may be necessary. This highlights the importance of a personalized approach when implementing EFT tapping as a therapeutic tool for non-verbal individuals, ensuring that each person’s unique needs and capabilities are adequately addressed.
Importance of Proper Training
Benefits of EFT training is essential for mental health professionals who aim to enhance their therapeutic skills and effectively address their clients’ emotional needs. The training process is structured in stages, beginning with an introductory externship followed by core skills training, which is crucial for refining practitioners’ abilities to understand and improve clients’ emotional literacy and overall well-being.
EFT training typically starts with a four-day foundation course known as an externship, which introduces participants to the basic concepts and applications of EFT. This is followed by core skills training, delivered in modules over several days or hours, focusing on deepening practitioners’ understanding of specific client groups. These training stages are designed to equip therapists with the necessary tools to clarify and address the emotional experiences of individuals, couples, and families effectively.
Moreover, becoming a certified EFT practitioner requires commitment to a person-centered or humanistic approach and an interest in expanding one’s professional toolkit. The training not only includes in-person workshops but also offers online modules to accommodate different learning preferences and geographical locations.
Advanced training modules are available for those who wish to specialize further, emphasizing the application of EFT in more complex cases or with specific demographics. These advanced courses are integral for practitioners who seek to enhance their expertise and adapt their therapeutic approaches to meet diverse client needs effectively.
The importance of ongoing professional development in EFT is underscored by the necessity to stay attuned to one’s own emotional states and vulnerabilities during therapy sessions. This self-awareness is crucial for maintaining an empathetic, yet professional, therapeutic relationship and for fostering an environment where clients feel safe to explore their emotions.
In summary, proper training in EFT not only enhances the therapeutic skills of mental health professionals but also supports their personal growth and the development of a nuanced understanding of human emotions. This comprehensive approach ensures that practitioners can provide effective and empathetic care, ultimately leading to better client outcomes.
Career Advancement Through EFT Training
Increased Earning Potential
Engaging in EFT Training can significantly boost your earning potential. By mastering the techniques taught in EFT Courses, you can offer specialized services that are in high demand, such as managing stress, anxiety, and emotional trauma.
Expanded Career Opportunities
Certification in EFT opens up a plethora of new career opportunities. There is a growing demand for certified EFT practitioners across various fields, including mental health, personal well-being, and holistic health.
Networking and Support
The EFT community offers invaluable networking opportunities. By attending an EFT Seminar or workshop, you can connect with other practitioners, learn from their experiences, and grow together.
Moving Beyond Medical Models
In the evolving landscape of mental health therapies, Emotional Freedom Technique (EFT) represents a significant departure from traditional medical models, emphasizing holistic and integrative approaches. Reviews and meta-analyses validate EFT as an evidence-based practice, with its efficacy for conditions such as anxiety, depression, phobias, and PTSD well-established. This recognition challenges the conventional reliance on pharmaceutical interventions by highlighting a noninvasive, nondrug therapy that is free of negative side effects and capable of inducing profound physiological and psychological changes.
Furthermore, the application of EFT in clinical settings has demonstrated its versatility and effectiveness across a wide range of psychological and physical symptoms, making it a valuable addition to existing treatment protocols. Despite some criticisms labeling EFT as pseudoscience, the technique continues to gain traction within the therapeutic community, particularly among those seeking non-traditional methods that align with a holistic view of health.
Critiques of EFT often focus on the lack of rigorous scientific research supporting its mechanisms. However, proponents argue that the simplicity of the technique, coupled with its ability to be self-administered, makes it an accessible option for those disillusioned with conventional treatments. This perspective is bolstered by the growing interest in energy psychology, which integrates established clinical methods with somatic interventions like tapping acupoints, showing strong effect sizes in treating PTSD, anxiety, and depression.
As mental health paradigms shift towards more integrative and person-centered approaches, EFT stands out as a modality that not only addresses the symptoms but also empowers individuals to actively participate in their healing process. This shift is indicative of a broader movement in healthcare, which increasingly values treatments that are not only effective but also enhance the overall quality of life by respecting the interconnectedness of mind, body, and spirit.
EFT Tapping Sessions Explained
 EFT (Emotional Freedom Techniques) tapping sessions are structured to help individuals address specific emotional issues by tapping on designated meridian points on the body. At the start of an EFT session, the practitioner asks the individual to think about the issue they wish to address and to rate the intensity of their emotions on a scale from 0 to 10, known as the Subjective Units of Distress (SUD) score. This initial assessment helps both the practitioner and the client gauge the emotional impact of the issue and track progress throughout the session.
EFT (Emotional Freedom Techniques) tapping sessions are structured to help individuals address specific emotional issues by tapping on designated meridian points on the body. At the start of an EFT session, the practitioner asks the individual to think about the issue they wish to address and to rate the intensity of their emotions on a scale from 0 to 10, known as the Subjective Units of Distress (SUD) score. This initial assessment helps both the practitioner and the client gauge the emotional impact of the issue and track progress throughout the session.
During the session, both the practitioner and the client tap on specific points on the face and torso, which are the endpoints of the body’s energy meridians. This process is aimed at alleviating emotional distress associated with negative memories or events without the need to dwell on the painful details. Clients are encouraged to focus on a negative event or memory while tapping, which helps to discharge the emotional charge linked to those thoughts, making the memory less triggering.
As the session progresses, the practitioner may guide the client to uncover and address various aspects of a specific event or unresolved emotion. This might include sensory details like sights, smells, or sounds associated with the memory. Each aspect is addressed thoroughly until the emotional charge is significantly reduced or eliminated.
Additionally, the practitioner might explore core beliefs or statements related to the client’s goals, such as losing weight or improving financial stability. The client is asked to rate how true these statements feel on a scale from 0 to 10, a measure known as the Validity of Cognition (VOC) score. If there is incongruence in these beliefs, tapping techniques are used to realign the subconscious beliefs with the client’s goals, enhancing their ability to achieve desired outcomes.
EFT sessions can be conducted in various formats, including in-person, over the phone, or via video conferencing platforms like Zoom or Skype, providing flexibility and access to clients regardless of geographical location. This adaptability makes EFT a practical tool for emotional management and self-regulation, accessible to a broad audience seeking relief from psychological distress.
Enhancing Therapeutic Skills
Improved Emotional Intelligence
Training in Emotionally Focused Therapy (EFT) significantly enhances a therapist’s emotional intelligence. This advanced understanding allows therapists to better recognize and interpret their clients’ emotional states, leading to more effective therapeutic interventions. By honing these skills, therapists can foster deeper connections and facilitate meaningful emotional growth in their clients.
Effective Stress and Anxiety Management
EFT training equips therapists with sophisticated techniques to manage stress and anxiety in their clients. These methods help in identifying the root causes of stress and anxiety, enabling therapists to address these issues more effectively. As a result, clients experience a reduction in their symptoms and an overall improvement in their mental health.
Advanced Techniques for Emotional Trauma
Therapists trained in EFT are adept at handling emotional trauma. They employ advanced techniques to help clients process and heal from traumatic experiences. This specialized training ensures that therapists can provide the necessary support and guidance, leading to significant emotional recovery and resilience in their clients.
Strengthening Personal Relationships
Building Secure Attachment Bonds
EFT aids individuals in recognizing and understanding the emotional drivers behind their actions, which can fortify their emotional ties with partners or family members. This process fosters more rewarding and supportive relationships.
Improved Communication Skills
By addressing the core emotions that cause relationship distress, clients can achieve greater emotional security and enhanced communication. This leads to deeper intimacy and a more satisfying relationship.
Conflict Resolution Strategies
EFT empowers clients to develop healthier interaction patterns with their loved ones. They learn to move away from destructive communication habits and adopt more constructive, secure, and emotionally fulfilling ways of relating.
Integrating with Other Modalities
Integrating Emotional Freedom Techniques (EFT) with other modalities enhances its effectiveness and provides a more holistic approach to emotional wellness. EFT, a versatile energy psychology technique, can be seamlessly combined with various therapies such as cognitive behavioral therapy, Reiki, and aromatherapy to address a wide range of emotional and physical issues.
For individuals who may not initially be ready for EFT due to their emotional state, starting with gentler therapies like Reiki or Flower Essences can prepare them for EFT. This approach ensures that each therapy complements the other, addressing different aspects of the body’s subtle energies. For instance, while EFT focuses on meridian points to balance the body’s energy system, Flower Essences target specific emotional states, enhancing the emotional healing process initiated by EFT tapping.
Moreover, integrating EFT with therapies like music, light, and color therapies can improve the overall therapeutic environment, making it more conducive to healing. This is particularly beneficial in cases where the sensory experience of tapping might be overwhelming for sensitive individuals. In such scenarios, the combination of EFT with other non-invasive therapies can soothe the nervous system and facilitate a more effective healing process.
Practitioners have found that using EFT in conjunction with established psychological therapies like psychotherapy and cognitive behavior therapy not only accelerates progress but also helps clients achieve a deeper emotional and psychological understanding. This integration allows therapists to use a hybrid knowledge base to inform their clinical choices, offering a comprehensive treatment approach that considers both emotional and cognitive aspects of wellness.
In conclusion, the integration of EFT with other modalities offers a multifaceted approach to therapy that addresses various dimensions of a person’s well-being. This method not only enhances the effectiveness of EFT but also empowers individuals with a variety of tools to manage their emotional health, promoting a more balanced and fulfilling life.
Diverse Applications of EFT
EFT for Individuals
Emotionally Focused Therapy (EFT) offers significant benefits for individuals by enhancing emotional awareness and self-regulation. What is EFT? It is a short-term, evidence-based intervention that helps people achieve a more authentic sense of self.
EFT for Couples
EFT is widely used in couples therapy to improve emotional bonds and communication. It is effective in various settings, including private practices and hospital clinics, and has been adapted for different cultures globally.
EFT for Families
EFT can also be applied to family therapy, helping to resolve conflicts and build stronger emotional connections among family members. This approach fosters a deeper understanding of emotional dynamics within the family unit.
Continuous Professional Development
Ongoing Learning Opportunities
Engaging in EFT training ensures that practitioners have access to a wealth of resources and continuous learning opportunities. This commitment to ongoing education helps therapists stay at the forefront of their field.
Access to EFT Workshops and Seminars
Participating in workshops and seminars allows EFT practitioners to deepen their understanding and refine their skills. These events provide a platform for learning the latest techniques and methodologies in EFT.
Staying Updated with Latest Research
Remaining informed about the latest research and advancements in EFT is crucial for any practitioner. This knowledge not only enhances their practice but also ensures they provide the most effective therapy to their clients.
Emotional and Mental Well-being
Achieving Emotional Equilibrium
Engaging in EFT training can significantly enhance one’s ability to maintain emotional balance. This therapeutic approach fosters a deeper understanding of personal emotions, enabling individuals to navigate their feelings more effectively.
Enhancing Self-Regulation
Through EFT, practitioners develop improved self-regulation skills. This means they can better manage their emotional responses, leading to greater impulse control and overall emotional stability.
Promoting Inner Serenity
EFT training also contributes to inner peace by helping individuals process and resolve emotional conflicts. This promotes a sense of calm and well-being, essential for mental health.
Conclusion
Through a comprehensive exploration of Emotional Freedom Techniques (EFT), this article has underscored the significant impact that EFT can have on emotional wellness and mental health. By integrating cognitive behavioral therapy elements with traditional Chinese acupressure, EFT emerges as a potent tool for addressing a broad spectrum of emotional distresses, from anxiety and depression to trauma and stress, enhancing overall quality of life. The accessibility and simplicity of the EFT tapping technique empower individuals to actively participate in their own healing process, offering a sense of autonomy and efficacy in managing personal emotional challenges. Moreover, the discussions on the necessity of proper training for practitioners, the benefits of EFT for non-verbal individuals, and its integration with other therapeutic modalities further delineate the versatility and effectiveness of EFT in the broader landscape of therapeutic interventions.
In recognizing the holistic nature of emotional and physical wellness, the article illuminates the profound implications of adopting EFT within therapeutic practices and personal self-care routines. As we move beyond conventional medical models towards more integrative and person-centered approaches, EFT stands out as a non-invasive, effective method that respects the interconnectedness of mind, body, and spirit. The potential of EFT to complement existing modalities and provide accessible, effective relief from emotional distress positions it as a pivotal addition to the future of mental health therapy. Thus, whether as part of a practitioner’s toolkit or an individual’s self-help strategy, EFT offers a promising path toward emotional resilience, healing, and a more harmonious state of being.
FAQs
What is Emotionally Focused Therapy (EFT)?
EFT is a short-term, practical, and evidence-based intervention that aims to improve clients’ emotional awareness, expression, and self-regulation. The results are a more authentic sense of self and improved relationships.
Who can enroll in EFT training?
Training to become an EFT practitioner is open to licensed mental health professionals who are committed to a person-centered or humanistic approach and have an interest in enhancing their existing toolkit.
What are the benefits of becoming an EFT therapist?
Enrolling in a certified EFT course can be a game-changer for your career. It increases your earning potential, expands career opportunities, and helps in developing a deeper understanding of clients’ emotions.
Is there scientific evidence supporting EFT?
Yes, EFT is based on the neuroscience of attachment and has a strong scientific evidence base. Research shows its long-term benefits in improving emotional and relational health.
Can EFT be applied to different types of clients?
Yes, EFT offers distinct training paths for individuals, couples, and families. Each path is specialized to address the specific needs and dynamics of these different relational units.
How does EFT help in stress and anxiety management?
EFT helps in managing stress and anxiety by improving emotional awareness and self-regulation. It enables clients to recognize and express their emotional needs more effectively, fostering healthier relationships.
What are the advantages of using the Emotional Freedom Technique (EFT)?
The Emotional Freedom Technique, or EFT, offers several benefits as outlined in the EFT International’s Free Tapping Manual. These include alleviating certain types of physical pain, enhancing sleep quality and patterns, reducing cravings, boosting creativity, and improving overall performance.
How does EFT contribute to emotional stability?
EFT, also known as tapping or psychological acupressure, is a form of alternative treatment aimed at relieving physical and emotional distress. It operates on the principle that tapping specific points on the body can help balance your energy system, thereby treating pain and enhancing emotional stability.
Why is EFT therapy considered significant?
EFT therapy is crucial because it equips individuals with the skills to better recognize, comprehend, and manage their emotions. This not only aids in improving personal well-being but also enhances interpersonal relationships.
What health benefits does EFT provide?
The Emotional Freedom Technique (EFT) is a mental health therapy that involves tapping on certain pressure points located on the hands, wrists, head, and body. This technique is used to help control thoughts, manage stress, and regulate emotions, contributing to overall mental health and stability.
Research Articles:
Emotional Freedom Techniques for Childhood Sexual Abuse Survivors. Maria Isabel Soriano-Lemen, Et Al. Published: 2023-05-03 Page: 9-21
Issue: 2023 – Volume 43 [Issue 2]
Emotional Freedom Techniques (EFT) Tapping for Pediatric Emergency Department Staff During the COVID-19 Pandemic: Evaluation of a Pilot Intervention. Susanne M. Bifano, Et Al. Publication: Medical Acupuncture. Vol. 36, No. 2 Published Online: 10 April 2024
The effect of emotional freedom techniques (EFT) on postpartum depression: A randomized controlled trial. Neriman Güdücü, Et Al. EXPLORE
Volume 19, Issue 6, November–December 2023, Pages 842-850.
Emotional Freedom Technique (EFT): Tap to relieve stress and burnout. Suzan Blacher, Et Al. Journal of Interprofessional Education & Practice
Volume 30, March 2023, 100599