By – James M. Katz, BA
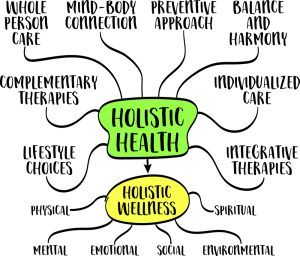
Holistic healthcare is transforming the way people approach their well-being. This comprehensive approach to health considers the whole person, integrating physical, mental, and spiritual aspects to promote overall wellness. As more individuals seek alternatives to traditional medical practices, holistic healthcare offers a unique perspective on healing and maintaining optimal health. Holistic wellness is a way of treating the whole person, not just the symptoms of a disease. It focuses on the balance of the body, mind, and spirit to achieve overall well-being. This guide will help you understand what holistic healthcare is, its benefits, and how you can use it in your life.
Holistic medicine emphasizes the connection between mind, body, and spirit, recognizing that each component plays a crucial role in a person’s health. This article explores the key concepts of holistic health, including integrative medicine approaches, nutrition and lifestyle factors, mental wellness techniques, and complementary therapies. It also delves into the practical implementation of holistic care in modern healthcare settings, providing insights into how this approach can enhance overall well-being and quality of life.
Key Takeaways
- Holistic healthcare treats the whole person, including body, mind, and spirit.
- It has a long history and includes practices like acupuncture, Ayurveda, and mind-body techniques.
- Holistic care can improve physical health, mental well-being, and help prevent illnesses.
- Integrating holistic healthcare with modern medicine can offer a more comprehensive approach to health.
- Choosing the right holistic healthcare provider involves checking their credentials and asking the right questions.
Understanding Holistic Healthcare
Definition of holistic healthcare
Holistic healthcare is a way of treating people that looks at the whole person, not just their illness. It focuses on the mind, body, and spirit. The main idea is that all parts of a person are connected. If one part is not well, it can affect the other parts. This type of care aims to find balance and wellness in all areas of life. While addressing the whole person, Holistic professionals consider physical, mental, emotional, social, and spiritual components of health. It goes beyond treating specific illnesses or symptoms, focusing on achieving a state of complete well-being. The World Health Organization defines health as “a state of complete physical, mental and social well-being and not merely the absence of disease or infirmity”. This definition aligns with the holistic perspective, emphasizing that true health encompasses more than just physical wellness.
Core principles
The core principles of holistic healthcare are rooted in the belief that all aspects of a person’s life are interconnected and influence overall health. Here are some key principles:
1. Treating the whole person: Holistic practitioners consider the entire individual, not just isolated symptoms or body parts.
2. Integration of conventional and alternative therapies: Holistic medicine combines traditional medical approaches with complementary and alternative therapies.
3. Prevention and self-care: Emphasis is placed on preventing illness and empowering patients to take an active role in their health.
4. Patient-practitioner relationship: A strong, collaborative relationship between the healthcare provider and patient is crucial for effective treatment.
5. Individualized care: Recognizing that each person is unique, holistic practitioners tailor treatments to the individual’s specific needs.
6. Healing power of nature: Holistic medicine acknowledges the body’s innate ability to heal itself and aims to support this natural process.
7. Education and empowerment: Patients are encouraged to learn about their health and make informed decisions about their care.
Historical background
Holistic healthcare has been around for a long time. Many ancient cultures, like those in China and India, used holistic methods to treat people. They believed that health was more than just not being sick. Over time, these ideas have spread and mixed with modern medicine.
The roots of holistic wellness can be traced back thousands of years to ancient healing traditions. Some notable historical aspects include:
1. Traditional Chinese Medicine (TCM): Originating nearly 5,000 years ago, TCM views the human body as a complex system of interconnected elements, including physical components and subtle energies like “qi” (life force) and “sheen” (spirit).
2. Ayurveda: This ancient Indian medical tradition, dating back to the 6th century B.C., incorporates beliefs in the five great elements of the universe and the three “doshas” or biological energies.
3. Western herbalism: Originating in ancient Greece and Rome, this practice spread throughout Europe and later to the Americas, focusing on the medicinal properties of plants and herbs.
4. Hippocrates: Known as the father of medicine in the 4th century B.C., Hippocrates emphasized the healing power of nature and encouraged self-healing efforts of the body.
The modern holistic health movement gained momentum in the late 1960s and early 1970s as a response to the limitations of conventional medicine. The first National Conference on Holistic Health was held in California in 1975, followed by the formation of the American Holistic Health Association (AHHA) and the Holistic Medical Association. Today, holistic healthcare continues to evolve, integrating evidence-based practices with traditional healing wisdom to provide comprehensive care for individuals seeking optimal health and well-being.
The Mind-Body Connection
Scientific Evidence
Recent research has shed light on the intricate connection between the mind and body, providing scientific evidence for what many have intuitively understood for centuries. A groundbreaking study published in the journal Nature reveals that parts of the brain controlling movement are directly linked to networks involved in thinking, planning, and regulating involuntary bodily functions. This discovery represents a literal linkage of body and mind within the very structure of the brain, offering a physiological basis for the mind-body connection.
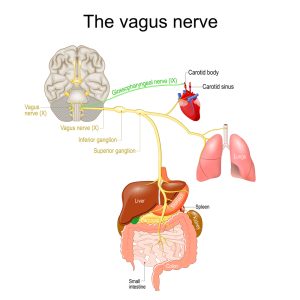
The findings help explain several phenomena that have long puzzled researchers. For instance, they provide insight into why anxiety often manifests as physical restlessness, why vague nerve stimulation may alleviate depression, and why regular exercise tends to improve mental well-being. These connections make sense when considering the brain’s primary function: to enable successful behavior in the environment while maintaining bodily integrity.
Psychoneuroimmunology
Psychoneuroimmunology (PNI) is a relatively new field of study that examines the interactions between the central nervous system (CNS) and the immune system. This emerging discipline has begun to unravel the complex communication pathways between these two crucial systems, providing valuable insights into how mental states can influence physical health and vice versa.
One key area of focus in PNI research is the role of cytokines, small proteins released by cells in the immune system. Studies have shown that both physical and psychological stress can trigger the release of pro-inflammatory cytokines. Under normal circumstances, these cytokines help combat infections and repair tissue damage. However, chronic stress can lead to prolonged elevation of these inflammatory markers, potentially contributing to various health issues.
Research has demonstrated that different types of stressors can elicit distinct cytokine responses. For example, physical injury may produce one type of pro-inflammatory cytokine, while social stressors, such as separation from a close family member, may trigger the release of a different type. This nuanced understanding of the stress response highlights the complexity of the mind-body connection and its far-reaching effects on health.
Stress and Its Effects
The impact of stress on the mind and body is profound and far-reaching. When faced with a stressful situation, the body initiates an automatic response, often referred to as the “fight-flight-freeze” response. This survival mechanism triggers the release of stress hormones like cortisol and adrenaline, preparing the body to face perceived threats.
While this response can be beneficial in short-term, acute stress situations, chronic stress can have detrimental effects on both mental and physical health. Ongoing stress has been linked to a wide range of symptoms, including headaches, sleep disturbances, digestive issues, and mood changes. Moreover, chronic stress has been associated with an increased risk of developing or exacerbating various major illnesses, such as heart disease, obesity, asthma, and autoimmune disorders.
The mind-body connection is particularly evident in the relationship between stress and mental health. Chronic stress has been shown to increase the risk of developing mental health conditions, including depression, anxiety disorders, and substance use disorders. This bidirectional relationship between mental and physical health underscores the importance of addressing stress through holistic approaches that consider both psychological and physiological factors.
Key Components of Holistic Healthcare
Physical Health
Physical health forms the foundation of holistic wellness. It involves maintaining a healthy lifestyle through regular exercise, consuming a balanced diet, getting adequate sleep, and managing stress. By prioritizing physical health, individuals can experience improved stamina, endurance, and overall well-being. This aspect of health not only impacts energy levels but also influences emotional and mental well-being.
A holistic approach to physical health examines the body’s needs for nutrition, sleep, exercise, and rejuvenation. It also considers the underlying causes of physical pain and explores steps to alleviate or cope with it. Additionally, it focuses on preventive measures to avoid bodily injury, illness, and disease.
Mental and Emotional Wellbeing
Mental and emotional health are integral components of holistic healthcare. Mental health encompasses psychological and cognitive well-being, involving the maintenance of a positive mindset, engagement in mental stimulation, and stress management. Good mental health is essential for problem-solving, decision-making, and interpersonal relationships. By fostering mental health, individuals can experience enhanced creativity, focus, and overall cognitive function.
Emotional health, on the other hand, is characterized by the ability to effectively manage emotions and maintain healthy relationships. It involves recognizing and expressing emotions, developing resilience, and fostering a strong support network. Emotional well-being allows individuals to better navigate life’s challenges and maintain overall mental health. Cultivating emotional intelligence and practicing empathy can lead to increased job satisfaction and improved interpersonal relationships.
When mental health is neglected, it can lead to various issues, including:
1. Poor physical health
2. Strained relationships
3. Decreased productivity
4. Lower quality of life
To promote mental and emotional well-being, individuals can:
1. Seek professional help when struggling with mental health issues
2. Develop healthy habits
3. Cultivate a strong support network
4. Practice mindfulness and relaxation techniques
5. Set realistic goals
Spiritual Aspects
Spirituality plays a crucial role in holistic healthcare, addressing the search for meaning, value, and connection. It involves recognizing, respecting, and meeting patients’ spiritual needs through various practices and approaches. Spiritual care can be implemented by facilitating religious or spiritual participation, supporting and showing empathy through listening and talking, and promoting a sense of well-being by helping individuals find meaning and purpose in their illness and life.
Spirituality has been strongly associated with resilience and quality of life across different cultures. Studies indicate that religion and spirituality are protective factors against depression and assist in recovery. Substantial evidence suggests positive associations between spirituality and longevity, reduced substance misuse, quicker healing after surgery, cancer recovery, and chronic pain management.
For individuals who do not identify as “religious,” clinicians can educate patients about complementary and integrative health approaches such as meditation, yoga, tai chi, listening to sacred music, and spending time in nature. Many of these approaches are preventative and cost-effective.
By addressing physical health, mental and emotional well-being, and spiritual aspects, holistic healthcare aims to optimize overall health and create a harmonious balance between various aspects of an individual’s life. This comprehensive approach recognizes the interconnectedness of these components and their collective impact on a person’s well-being.
Integrative Medicine Approaches
Integrative medicine is an approach that combines conventional medical practices with complementary and alternative therapies to treat the whole person – mind, body, and spirit. This holistic approach has gained significant traction in recent years, with a growing number of healthcare institutions incorporating integrative medicine into their services.
Combining conventional and alternative therapies
Integrative medicine seeks to blend the best of both worlds by utilizing evidence-based conventional treatments alongside complementary therapies. This approach recognizes that a patient’s physical, emotional, mental, and spiritual needs are interconnected and affect overall well-being. By integrating various therapies, healthcare providers aim to achieve optimal health and healing for their patients.
Some common complementary therapies used in integrative medicine include:
1. Acupuncture
2. Yoga
3. Chiropractic care
4. Meditation
5. Herbal medicine
The integration of these therapies with conventional medicine has become increasingly prevalent. A survey conducted in 2001 revealed that 15% of hospitals offered complementary and alternative medicine (CAM) services, more than doubling from 6% in 1998. This trend indicates a growing interest in holistic approaches to healthcare.
Evidence-based practices
Integrative medicine emphasizes the use of evidence-based practices to ensure the safety and effectiveness of treatments. This approach aligns with the scientific method and evidence-based medicine, which focus on objectively verifiable criteria to evaluate the efficacy of various therapies.
Healthcare providers practicing integrative medicine consider a wide range of factors that influence health, wellness, and disease, including the mind, spirit, and community, as well as the body. They aim to use natural, less invasive interventions whenever possible while remaining open to new paradigms and inquiry-driven approaches.
Patient-centered care
A cornerstone of integrative medicine is patient-centered care, which focuses on treating the individual rather than just the disease. This approach recognizes that each patient is unique and requires personalized care that addresses their specific needs and preferences.
Patient-centered care in integrative medicine includes the following dimensions:
1. Respect for patient preferences
2. Coordination and integration of care
3. Information and education
4. Physical comfort
5. Emotional support
6. Involvement of family and friends
7. Continuity and transition
8. Access to care
By adopting a patient-centered approach, integrative medicine practitioners aim to establish a partnership with their patients in the healing process. This collaboration empowers patients to take an active role in their health and well-being, leading to improved outcomes and higher patient satisfaction.
Integrative medicine practitioners work alongside conventional healthcare providers, complementing rather than replacing primary care or specialist services. Their expertise lies in preventing and managing chronic diseases, focusing on long-term health and wellness rather than acute medical problems.
As integrative medicine continues to evolve, it offers a promising approach to healthcare that addresses the complex needs of patients in today’s world. By combining the best of conventional and complementary therapies, utilizing evidence-based practices, and focusing on patient-centered care, integrative medicine strives to provide comprehensive, holistic care that promotes optimal health and healing.
Nutrition and Lifestyle in Holistic Health
Whole foods and diet
Whole foods plant-based approaches to eating have gained significant attention in holistic health practices. These diets emphasize the consumption of fruits, vegetables, whole grains, and legumes, offering numerous health benefits. One of the primary advantages of whole foods is their nutritional density, providing essential vitamins, minerals, and antioxidants.
Whole foods plant-based diets are particularly rich in dietary fiber and phytochemicals, including carotenoids, flavonoids, isothiocyanates, lignans, phytosterols, and stilbenes. Dietary fibers, which are nondigestible carbohydrates and lignans naturally occurring in plant-based foods, offer various health benefits such as cardiovascular disease risk reduction, diabetes control, and improved laxation. However, it’s worth noting that the average intake of dietary fiber among US adults is only 16 grams per day, falling short of the recommended 28 grams for an adult consuming 2000 kcal per day.
While whole foods plant-based diets offer numerous advantages, it’s important to be aware of potential nutrient deficiencies. Research has identified key nutrients that individuals following these dietary patterns may be at risk for inadequate intake, including calcium, iron, vitamin D, omega-3 fatty acid (DHA), and vitamin B12. To address these concerns, individuals can incorporate calcium-fortified foods, plant-based iron sources, and consider dietary supplements when necessary.
Exercise and movement
Physical activity plays a crucial role in holistic health, offering benefits for both physical and mental well-being. Regular exercise can help manage chronic pain, reduce fatigue, improve sleep quality, and enhance mood. Research indicates that physical activity can reduce anxiety, mitigate depression, and help balance mood.
Incorporating wellness exercises into holistic treatment plans can complement evidence-based medical treatments. Mind-body practices such as movement therapy, which includes techniques like breathing exercises, yoga, tai chi, qi gong, and dance, focus on body awareness and mindfulness to help cope with pain.
For older adults, staying active is particularly important. Studies show that inactivity, rather than age, is often responsible for the loss of independence in older individuals. Regular physical activity can help maintain and improve strength, increase energy levels, and reduce the risk of falls and injuries.
Sleep and rest
Adequate sleep is a fundamental aspect of holistic health, playing a vital role in both physical and mental well-being. Quality sleep promotes wellness, and wellness, in turn, promotes better sleep. During sleep, the brain consolidates memories and undergoes maintenance processes essential for daytime functioning.
Sleep offers numerous benefits, including improved memory consolidation, increased concentration, reduced stress, and enhanced physical health. It also plays a role in regulating hormones, including those responsible for libido.
To improve sleep quality, it’s important to create an accommodating sleep environment free from intrusive noise, light, and heat. Establishing a consistent sleep routine can support the body’s biological clock, preparing it for rest. It’s also advisable to limit exposure to digital screens before bedtime, as the blue light they emit can disturb melatonin production and interfere with drowsiness.
For those struggling with sleep issues, cognitive behavioral therapy (CBT) has been shown to be an effective treatment, even for long-term insomnia. This approach can help establish good sleep patterns and develop a healthy mental outlook towards sleep.
Mental and Emotional Wellness Techniques
Mindfulness and Meditation
Mindfulness and meditation are powerful techniques for promoting mental and emotional well-being. Mindfulness involves increasing awareness of the present moment by focusing on thoughts, feelings, and sensations. This practice can help reduce stress, improve focus, and encourage mental growth. Meditation, which often incorporates mindfulness, can provide a sense of calm, peace, and balance that benefits emotional well-being and overall health.
There are various mindfulness and meditation techniques:
1. Focused attention: This involves concentrating on a specific object, thought, or action to free the mind from stress and worry.
2. Relaxed breathing: Deep, even-paced breathing using the diaphragm muscle can slow breathing, increase oxygen intake, and reduce tension. https://www.mayoclinic.org/tests-procedures/meditation/in-depth/meditation/art-20045858
3. Body scan meditation: Also known as progressive relaxation, this technique involves systematically focusing awareness on different parts of the body.
4. Walking meditation: Practiced at a leisurely pace, this method encourages focusing on bodily sensations, surroundings, and breath.
5. Mantra repetition: Internally or verbally reciting a mantra, phrase, or intention can help calm the mind and encourage concentration.
Regular practice of mindfulness and meditation can lead to improved emotional regulation, reduced symptoms of anxiety and depression, and increased calmness, patience, and empathy.
Cognitive Behavioral Therapy
Cognitive Behavioral Therapy (CBT) is a pivotal component in holistic mental health care. It focuses on the interconnection between thoughts, feelings, and behaviors. CBT aims to change automatic negative thoughts that contribute to emotional difficulties, depression, and anxiety.
Key aspects of CBT include:
1. Identifying and challenging negative thought patterns
2. Understanding and reshaping core beliefs
3. Developing healthier cognitive patterns for long-term wellness
4. Breaking down overwhelming problems into smaller, manageable components
CBT empowers individuals to transform destructive thought patterns into ones that promote balance and health. By addressing both cognitive and behavioral aspects, CBT provides a comprehensive approach to mental health care.
Stress Management
Effective stress management is crucial for maintaining mental and emotional wellness. Chronic stress can lead to various physical and psychological issues, including depression, anxiety, heart disease, and sleep disturbances.
Holistic approaches to stress management include:
1. Nutrition: Eating protein-rich meals at regular intervals helps balance blood sugar levels, reducing stress on the adrenal glands.
2. Gut health: Consuming fermented foods introduces probiotics to the gut, which can assist in reducing anxiety.
3. Omega-3 fats: Adequate intake of EPA and DHA plays an important role in adrenal health and brain behavior.
4. Hydration: Drinking 6-8 glasses of pure filtered water daily supports adrenal health.
5. Exercise: Engaging in physical activity at least three times a week can significantly improve stress management.
6. Meditation: Practicing meditation for as little as 10 minutes a day can have profound effects on stress reduction.
By incorporating these techniques into daily life, individuals can develop a holistic approach to mental and emotional wellness, fostering resilience and promoting overall well-being.
Complementary and Alternative Therapies
Complementary and alternative therapies encompass a wide range of practices that are used alongside or in place of conventional medicine. These therapies aim to promote holistic health and well-being by addressing the interconnectedness of mind, body, and spirit. Three prominent complementary and alternative therapies are acupuncture, herbal medicine, and energy healing.
Acupuncture
Acupuncture is an ancient practice rooted in Traditional Chinese Medicine (TCM) that has gained recognition worldwide. This therapy is based on the belief that the body’s vital energy, known as qi, flows through specific channels or meridians. Practitioners insert thin needles into specific points along these meridians to restore balance and promote healing.
Studies have shown that acupuncture can be effective in treating various conditions, including:
1. Nausea caused by surgical anesthesia and cancer chemotherapy
2. Dental pain after surgery
3. Headaches and migraines
4. Menstrual cramps
5. Osteoarthritis
6. Low back pain
7. Carpal tunnel syndrome
Acupuncture is believed to stimulate the central nervous system, releasing chemicals that may promote physical and emotional well-being. While its effectiveness has been demonstrated for certain conditions, it’s important to consult with a healthcare provider before starting acupuncture treatment.
Herbal Medicine
Herbal medicine, also known as botanical medicine or phytomedicine, involves using plants or plant extracts for medicinal purposes. This practice has a long history, with ancient Chinese and Egyptian writings describing medicinal uses for plants as early as 3,000 BC.
Key aspects of herbal medicine include:
1. Widespread use: The World Health Organization estimates that [80% of people worldwide rely on herbal medicines for some part of their primary health care]
2. Pharmaceutical influence: Almost one-fourth of pharmaceutical drugs are derived from botanicals.
3. Regulation: In the United States, herbal supplements are classified as dietary supplements and are not subject to the same rigorous testing as prescription drugs.
Herbal medicine is used to treat various conditions, including allergies, asthma, eczema, premenstrual syndrome, and chronic fatigue. However, it’s crucial to consult with a healthcare provider before using herbal supplements, as they can interact with conventional medications and may have side effects.
Energy Healing
Energy healing is based on the belief that the human body encompasses an energetic “life force” and energy centers (chakras) that influence overall health. This practice aims to restore balance and harmony within the body’s energy systems.
Common energy healing modalities include:
1. Reiki
2. Light Therapy
3. Acupuncture
4. Reflexology
5. Thai Massage
6. Tapping
Energy healing practitioners believe that by channeling universal life force or healing energy into a patient, they can help remove blockages and restore vitality. While scientific evidence supporting energy healing is limited, proponents argue that it can complement conventional medical treatments.
It’s important to note that energy healing should not replace Western medicine but can be used in conjunction with conventional treatments to support overall well-being. As with any complementary therapy, individuals should consult with their healthcare providers before incorporating energy healing into their health regimen.
Implementing Holistic Healthcare
Working with practitioners
Implementing holistic healthcare involves collaborating with professionals who look beyond traditional Western medicine to offer a comprehensive approach to wellness. Holistic health practitioners consider all aspects of an individual’s well-being, including physical, emotional, mental, and spiritual health. These professionals use a variety of techniques, such as bodywork, nutrition, herbs, mindfulness, and other healthful practices, to help clients achieve optimal health and balance in life.
When working with holistic health practitioners, patients can expect a thorough evaluation of their health, including medical history, current health status, and lifestyle. This comprehensive assessment allows practitioners to develop personalized treatment plans that address the unique needs of each individual.
Creating a personalized plan
A personalized holistic wellness plan is designed to address all aspects of an individual’s well-being. Unlike generic programs, these plans are custom-crafted to align with specific health goals, challenges, and preferences. They take into account various factors such as age, fitness level, dietary preferences, stress factors, medical history, and even genetic makeup.
Key components of a personalized holistic wellness plan may include:
1. Customized exercise programs
2. Tailored dietary recommendations
3. Stress management techniques
4. Mental and emotional wellness strategies
5. Social interaction and community involvement
6. Guidance on sustainable lifestyle changes
The plan may also incorporate consultations with specialists such as nutritionists, personal trainers, or therapists as required. By addressing all areas of life, these plans can lead to a more profound and sustainable improvement in overall well-being.
Long-term lifestyle changes
Implementing holistic healthcare involves making long-term lifestyle changes that promote overall well-being. These changes are designed to instill lifelong habits and behaviors that support continuous health and happiness. Some key aspects of long-term lifestyle changes include:
1. Stress management: Incorporating techniques such as mindfulness exercises, meditation, and breathing techniques to manage stress more effectively.
2. Emotional resilience: Developing emotional resilience through cognitive-behavioral therapy (CBT) and positive psychology to better manage difficult emotions and maintain a positive outlook.
3. Mental clarity: Engaging in activities that promote mental clarity and focus, such as brain-training exercises, journaling, or creative hobbies.
4. Social connections: Fostering social interactions and connections with like-minded individuals to support overall well-being.
5. Preventive care: Emphasizing prevention and maintenance of health, rather than solely reacting to health issues as they arise.
By adopting these long-term lifestyle changes, individuals can take a more active role in managing and maintaining their health, leading to fuller, more productive lives. It’s essential to remember that implementing holistic healthcare is an ongoing process, and the plan should evolve as an individual’s needs change, ensuring that it remains effective and applicable to their current situation.
Holistic Healthcare for Different Life Stages
Children and Adolescents
Holistic healthcare for children and teens focuses on their unique needs as they grow. It includes natural treatments and lifestyle changes to support their physical, mental, and emotional development. Parents often seek holistic care to avoid the side effects of conventional medicine. This approach can help with common issues like allergies, ADHD, and stress.
Adults and Seniors
For adults and older people, holistic healthcare aims to maintain balance and prevent illness. It combines traditional medicine with alternative therapies to improve overall well-being. This can include practices like acupuncture, yoga, and herbal remedies. Many adults turn to holistic methods to manage chronic conditions and improve their quality of life.
Special Considerations for Pregnancy
During pregnancy, holistic healthcare offers gentle and safe options for both the mother and the baby. It focuses on nutrition, stress reduction, and natural remedies to support a healthy pregnancy. Expectant mothers often choose holistic care to avoid medications that might affect their baby. Techniques like prenatal yoga and acupuncture can help with common pregnancy issues like nausea and back pain.
Holistic Healthcare and Lifestyle
Nutrition and Diet
Eating well is a big part of staying healthy in holistic healthcare. A balanced diet can help your body work better and keep you feeling good. Fresh fruits, vegetables, whole grains, and lean proteins are often recommended. Avoiding processed foods and sugary drinks can also make a big difference.
Exercise and Physical Activity
Staying active is another key part of a holistic lifestyle. Regular exercise can boost your mood, improve your energy levels, and help you sleep better. Activities like walking, yoga, and swimming are great choices. Even small changes, like taking the stairs instead of the elevator, can add up over time.
Stress Management Techniques
Managing stress is important for your overall well-being. Techniques like deep breathing, meditation, and spending time in nature can help you relax. Finding what works best for you can make a big difference in how you feel every day. Taking time for yourself and doing things you enjoy can also help reduce stress.
Future Trends in Holistic Healthcare
Technological Innovations
The future of holistic healthcare is being shaped by new technologies. Wearable devices and mobile apps are making it easier for people to track their health and wellness. These tools help people stay on top of their physical and mental health, offering real-time data and personalized advice.
Research and Evidence-Based Practices
As more studies are done, the benefits of holistic healthcare are becoming clearer. Researchers are finding new ways to prove that these methods work. This helps more people trust and use holistic healthcare. It also helps doctors and other healthcare providers feel more confident in recommending these practices.
Global Perspectives
Holistic healthcare is growing all over the world. Different cultures bring their own ideas and methods to the table. This mix of global practices helps create a richer and more effective approach to health and wellness. By learning from each other, we can find the best ways to stay healthy and happy.
Conclusion
Holistic healthcare offers a comprehensive approach to well-being that has an impact on individuals seeking alternatives to traditional medical practices. By addressing physical, mental, and spiritual aspects of health, this approach aims to promote overall wellness and enhance quality of life. The integration of conventional medicine with complementary therapies, along with a focus on nutrition, lifestyle, and mental well-being, provides a well-rounded strategy to maintain health and prevent illness.
As holistic healthcare continues to evolve, it presents exciting opportunities to improve healthcare outcomes and empower individuals to take charge of their well-being. By working closely with healthcare practitioners and creating personalized plans, people can make lasting lifestyle changes that support their health goals. This holistic approach not only has the potential to enhance individual health but also to transform the broader healthcare landscape, encouraging a more balanced and comprehensive view of wellness.
If you’re interested in receiving training in holistic healthcare then you should review our Holistic and Integrative Healthcare Program. This program is only available to Registered Nurses or a higher level nursing license. It consists of 6 online holistic nursing courses. All of our courses are on open enrollment and self-paced, meaning you start whenever you’re ready and move through them at your own speed. If you would care to visit our online holistic nursing courses, please click the here.
FAQs
- What is holistic healthcare?
Holistic healthcare is a way of treating people that looks at the whole person. It focuses on the body, mind, and spirit to help people stay healthy.
- How is holistic healthcare different from traditional medicine?
Traditional medicine often treats just the symptoms of a disease. Holistic healthcare looks at the root cause and aims to improve overall well-being.
- What are some common holistic healthcare practices?
Some common practices include acupuncture, herbal medicine, and mind-body techniques like yoga and meditation.
- Can holistic healthcare be combined with regular medical treatments?
Yes, many people use holistic healthcare along with traditional treatments. This can help improve overall health and well-being.
- How do I choose a holistic healthcare provider?
Look for providers with the right credentials and qualifications. Ask questions about their experience and make sure you feel comfortable with them.
- Are there any risks to holistic healthcare?
While many holistic practices are safe, some may have risks. It’s important to talk to a healthcare provider before starting any new treatment.
- What does holistic care encompass?
Holistic care involves treating the entire individual, addressing the physical, mental, spiritual, and social needs. This approach is based on the understanding that each of these aspects influences overall health, and an issue in one area can impact the others.
- What are the main elements of holistic care?
Holistic care focuses on the whole person, which includes physical, emotional, mental, social, spiritual, and financial health. By considering all these dimensions, the approach aims to achieve the healthiest and happiest state of an individual.
- What are the five key areas of holistic health?
Holistic health covers five primary areas: Mental Health, Physical Health, Spiritual Health, Intellectual Health, and Social Health. These areas are integral to the holistic approach to health and wellness.
- What are the five pillars of holistic health care?
The five main pillars of holistic health include Physical Health, which is often the most recognized aspect of health; Mental and Emotional Health, which focuses on psychological well-being; Social Health, which pertains to how we interact and form relationships; Environmental Health, which involves the surroundings that affect our health; and Spiritual Health, which deals with our sense of purpose and overall well-being.
Research Articles:
The effect of biopsychosocial holistic care models on the cognitive function and quality of life of elderly patients with mild cognitive impairment: a randomized trial.
Li-Li Gong Et Al. APM. Vol 10, No 5 (May 29, 2021)
Access link here
A Holistic Examination of Patient Outcomes, Healthcare Accessibility, and Technological Integration in Remote Healthcare Delivery.
Haritha Atluri, Bala Siva Prakash Thummisetti. Transactions on Latest Trends in Health Sector Vol 14, No 14 (2022)
Access link here
Mitigating language and cultural barriers in healthcare communication: Toward a holistic approach. Barbara C. Schouten, Et Al. Patient Education and Counseling. Volume 103, Issue 12, 2020, Pages 2604-2608, ISSN 0738-3991,
Access link here
Towards Holistic Healthcare: Integrating Traditional and Modern Medicine for Improved Patient Outcomes. Kustiyati, S., Fajri, I. K., Masithoh, R. F., Dewi, R. D. C., & Nurseha, N. (2024). Global International Journal of Innovative Research, 2(5), 942–951.
Access link here













 The future of meditation in holistic nursing is bright, with many chances for new research. Studies can explore how meditation helps different patient groups and conditions. Research can also look at how meditation affects long-term health and recovery. This will help nurses use meditation more effectively in their care plans.
The future of meditation in holistic nursing is bright, with many chances for new research. Studies can explore how meditation helps different patient groups and conditions. Research can also look at how meditation affects long-term health and recovery. This will help nurses use meditation more effectively in their care plans.











