 Written by Nadine Westwood
Written by Nadine Westwood
Healthcare is one of the fastest-changing (and fastest-growing) industries. Just take a look at the rate at which medical knowledge evolves – what was considered best practice just a decade ago might now be outdated or even dangerous in some cases.
The way we diagnose, treat, and interact with patients is constantly being shaped by new research, emerging technologies, and evolving healthcare policies. This all to say, if you’re not actively learning, you’re falling behind.
Mind you, continuing education in healthcare isn’t just about meeting licensure requirements or adding a certification to your résumé (although this can only help your professional development). What this is about, is maintaining clinical excellence, ensuring ethical integrity, and staying adaptable in a rapidly evolving industry.
In this article, we explore why continuous learning is critical for every healthcare professional, explaining how it enhances your clinical skills, broadens career opportunities, and ultimately improves patient outcomes. We also look at practical ways to integrate ongoing education into your probably already demanding schedule without compromising your work-life balance.
The Rapid Evolution of Healthcare Demands Constant Learning
Medical advancements happen fast. According to research, the amount of medical knowledge in 1950 doubled approximately every 50 years. By 2020, it was doubling every 73 days. That means if you graduated from medical school a few years ago and haven’t engaged in continued learning, a significant portion of what you once knew may now be outdated.
Take a look at artificial intelligence (AI) in diagnostics. AI-driven imaging tools now detect early-stage cancers with the same accuracy as experts. Precision medicine, on the other hand, is transforming treatment plans by tailoring therapies to individual genetic profiles.
And robotic-assisted surgeries are becoming more ubiquitous and refined, allowing for minimally invasive procedures with faster recovery times. Keeping up with these developments is essential for any healthcare professional.
In addition to technology, patient care models are evolving, too. The shift from volume-based to value-based care means a greater emphasis on patient outcomes, interdisciplinary collaboration, and preventive medicine. The key is to keep updating these skills; otherwise, you risk falling out of sync with modern healthcare priorities.
Advancing Clinical Skills Through Ongoing Education
Whether you’re a physician, nurse, therapist, or allied health professional, clinical skills require continuous refinement, making continuing education a must. Here’s how it can help you expand expertise in ways that directly impact patient care:
- Improving diagnostic accuracy: New tests and imaging techniques emerge regularly. Staying informed reduces diagnostic errors and improves early detection rates.
- Enhancing procedural skills: From laparoscopic advancements to non-invasive cardiac imaging, mastering new techniques improves efficiency and patient outcomes.
- Strengthening interdisciplinary collaboration: Healthcare increasingly relies on team-based care. Understanding the roles of other professionals – pharmacists, social workers, mental health specialists – is therefore crucial for improving coordination and patient safety.
- Refining patient communication: A well-informed patient is more likely to follow treatment plans. Training in patient-centered communication leads to better adherence, fewer complications, and higher satisfaction rates.
With ongoing education, you’ll be expanding your knowledge and making yourself more attractive to potential employers; without it, you’re limiting your professional growth and the quality of care you can provide.
Elevating Professional Credentials and Career Opportunities
Investing in continued education can lead to specialization, higher salaries, leadership positions, and even entirely new career paths within healthcare. Here’s how:
- Specialization and advanced certifications: Pursuing board certifications in areas like geriatrics, oncology, or emergency medicine sets you apart and increases your earning potential.
- Expanded career paths: With additional education, you can move into roles like hospital administration, public health policymaking, or academic instruction.
- Leadership potential: Healthcare institutions prioritize leaders who stay current with industry trends. Advanced degrees (such as an MHA or MPH) can prepare you for executive roles in healthcare organizations.
Also, it’s worth noting that many professional licenses require ongoing education to maintain certification. So whether you’re a registered nurse, physician, or physical therapist, staying compliant is essential, as it signals dedication to your profession.
The Role of Continuing Education in Ethical Practice
What’s crucial to understand is that medicine isn’t just about technical skills – it’s also deeply rooted in ethics. Ethical dilemmas arise regularly, from end-of-life care decisions to patient privacy concerns in an era of digital health records. What does this have to do with continuous education? Well, ongoing education is essential for staying well-versed in the ethical guidelines that govern your field.
For instance, the American Medical Association (AMA) updates its Code of Medical Ethics regularly. If you’re unaware of the latest changes, you may unintentionally breach ethical or legal standards. Courses in bioethics, cultural competency, and healthcare law help ensure that your practice aligns with evolving regulations and societal expectations.
Beyond compliance, ongoing education encourages reflective practice: constantly evaluating your own biases, behaviors, and decisions to uphold the highest standards of patient care.
Practical Ways to Pursue Ongoing Education
Balancing continuing education with an already demanding career can seem nearly impossible, but there are flexible ways to make it work:
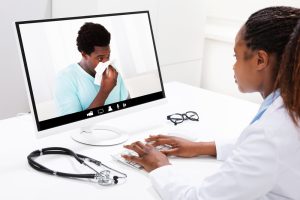
- Online courses and webinars: Many universities and professional organizations offer high-quality virtual learning options that can easily fit into busy and unpredictable schedules.
- In-person workshops and conferences: Attending industry events is perfect if your time allows it, as it allows for hands-on learning, networking with peers, and exposure to new ideas.
- Employer-sponsored training: Many healthcare institutions provide on-site education, mentorship programs, and tuition assistance for advanced degrees, so take advantage of it if possible.
- Medical journals and podcasts: Regularly reading reputable journals, like JAMA or The New England Journal of Medicine, or listening to medical podcasts is a great way to keep yourself updated on the latest developments without requiring formal coursework.
The point is, an all-or-nothing mentality isn’t helpful here. Small efforts, as long as they’re consistent, can have a significant impact on your knowledge and skills over time.
Balancing Education with Work and Personal Life
Most healthcare professionals already face high-pressure work environments. That’s why you want to add continuing education to the mix in a smart way, so it doesn’t lead to burnout but actually enhances your life:
- Prioritize learning goals: Identify what skills or knowledge gaps are most relevant to your role and start there.
- Integrate learning into daily routines: Listen to medical podcasts on your commute, read journal articles during breaks, or take short online courses on weekends.
- Leverage employer support: Many workplaces offer education stipends, flexible schedules, or paid study leave – take advantage of these resources.
- Set realistic expectations: Avoid overloading yourself. Continuous learning should enhance your career, not contribute to burnout.
- Create a structured plan: Setting specific goals, such as completing a certification within six months or attending a conference once a year, helps maintain progress without feeling overwhelmed.
- Find a support system: Engaging with peers who are also pursuing continuing education can provide motivation and accountability. Study groups, mentorship programs, or even online forums can be invaluable in maintaining momentum.
If you’re looking for guidance on balancing personal commitments with educational pursuits, platforms like Mind Body Dad offer valuable insights. Take advantage of free resources like this one to harmonize work, learning, and family life and ensure your career growth doesn’t come at the expense of personal well-being.
Remember, the goal isn’t to do everything at once, but to build a habit of lifelong learning that enhances your career without sacrificing your personal life.
Staying Ahead in a Competitive Field
Another important reason why you should commit to ongoing learning?
It can give you a significant strategic advantage. After all, the healthcare field is highly competitive, so if you want to position yourself for success, leadership roles, specialized opportunities, and career longevity, it’s crucial to invest in life-long learning. Employers actively seek professionals who demonstrate commitment to growth, plus patients benefit from providers who stay at the forefront of medical advancements.
Expanding your knowledge also helps you adapt to emerging trends. Telemedicine, artificial intelligence in diagnostics, and personalized medicine are reshaping healthcare, and professionals who fail to keep up risk becoming obsolete.
A 2024 report by McKinsey & Company highlighted how digital transformation in healthcare is accelerating, with an increasing demand for tech-savvy practitioners who can integrate new tools into patient care. By committing to ongoing education, you future-proof your career while enhancing patient outcomes.
Networking is another benefit. Attending conferences, enrolling in advanced courses, or participating in professional organizations connects you with leading minds in your field. These interactions open doors to collaborations, mentorships, and career advancements that wouldn’t be possible otherwise.
Whether you’re aiming for a promotion, a specialization, or simply to be the best in your field, continuing education is the key to staying relevant in a rapidly evolving industry.
The Bigger Picture: Why It Matters
At the center of continuing education is one fundamental truth: it directly impacts patient outcomes. The more knowledgeable and skilled you are, the better care you provide. But beyond individual benefits, lifelong learning elevates the entire healthcare system, leading to:
- More accurate diagnoses
- More effective treatments
- Stronger patient-provider relationships
- Improved public health initiatives
The commitment to ongoing education, therefore, separates great healthcare professionals from those who simply meet the minimum requirements. And in a field where lives are on the line, the choice to continue learning isn’t just professional, but one could argue ethical, as well.
Author bio:
Nadine Westwood is a health coach and writer who helps her clients achieve phenomenal and sustainable results by combining nutrition, fitness, education and fun!
References:
- 5 out of 20 fastest-growing industries from 2019 to 2029 are in healthcare and social assistance
- Challenges and Opportunities Facing Medical Education
- Dermatologist-level classification of skin cancer with deep neural networks
- Burnout and Workload Among Health Care Workers: The Moderating Role of Job Control
- Digital transformation: Health systems’ investment priorities
Please also review AIHCP’s Continuing Education Courses and see if it meets your academic and professional goals. These programs are online and independent study and open to qualified professionals seeking a four year certification





 Written by
Written by  By Lucy Peters,
By Lucy Peters,




 Written by Charles Schubert.
Written by Charles Schubert.





 Written by Charles Schubert
Written by Charles Schubert