Written by Veronica Turner
Written by Veronica Turner
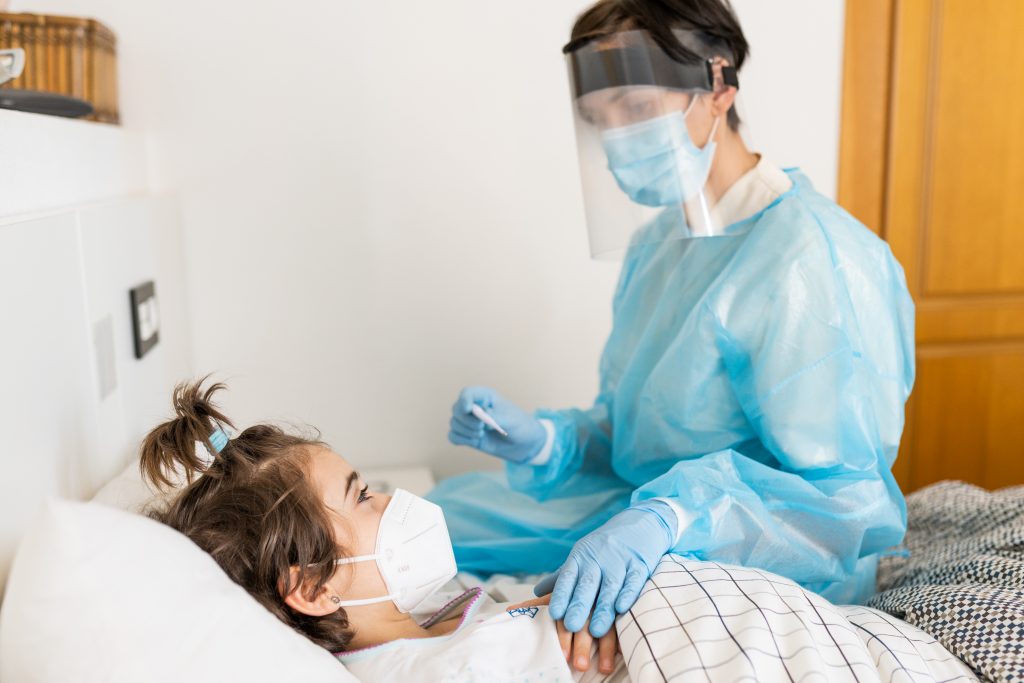
The effects of childhood illnesses can linger, shaping mental health for years to come.
For instance, chronic conditions like asthma or diabetes require frequent medical care and lifestyle adjustments, which can contribute to feelings of difference or exclusion. In turn, long-term mental health can be significantly impacted.
The Role of Early Bonds and Attachments
Childhood illnesses can majorly impact the development of early bonds and attachments, which are the foundation for future relationships.
A child constantly in medical care might have less opportunity to cultivate strong connections with peers or siblings. Over time, these disruptions can lead to difficulties in forming close relationships, potentially stimulating long-term feelings of loneliness or isolation.
This could then contribute to mental health problems such as depression and social anxiety disorders later in life.
Social Exclusion
Following on from the last point, social relations can take a hit when battling health issues during the early years.
Difficulty in keeping up with peers physically often leads to withdrawal from social activities or rejection by peer groups, which may trigger depression in later life stages.
Stress Factors
Dealing with illnesses in childhood can create an inherent level of stress. Often, that can result in anxiety symptoms as a reaction to the situation.
For example, fear of recurring symptoms or impending medical appointments can lead to prolonged periods of worry.
Impact on Self-Image and Identity
One of the profound long-term mental health impacts can be seen in the child’s developing self-image and identity.
Chronic illness might cause children to feel different or develop the perception that they are ‘abnormal’.
Over time, this negative self-image can lead to problems like body dysmorphic disorder or eating disorders.
Thus, addressing these distorted perceptions early is vital for preventing future mental health issues.
Psychological Effects
Dealing with physical discomfort and pain frequently plays out in one’s mental arena, affecting sufferers’ perceptions of self and overall satisfaction in life.
It’s not uncommon for such circumstances to lead to low self-esteem and a pessimistic worldview.
Impact on Education
Educational opportunities may be hampered by chronic sickness, as well.
In addition to the physical toll it takes, illness may cause cognitive impairments or interruptions in schooling that hinder academic progress.
Consequently, this educational disruption feeds into one’s mental well-being resulting in feelings of insecurity or dissatisfaction.
Long-Term Trauma
The traumatic experience of prolonged medical treatments during formative years can carve deep emotional scars and even lead to PTSD in some cases.
Also, the repeated pain and invasiveness related to certain treatments can leave lingering fears or aversions tied closely to one’s self-sense.
Resilience Development
There is a flip side. Some children who experience illnesses early in life develop extraordinary resilience over time.
In dealing with adversity at a young age, they may acquire coping skills that fortify them against future mental health challenges.
Therefore, outcomes are not always negative. Childhood illness can sometimes lead to heightened emotional robustness in adulthood.
The Importance of Professional Help
Entrusting mental well-being with professionals who specialize in child psychology becomes crucial when dealing with the aftermath of childhood ailments.
The intervention of experts at an early stage can help individuals to manage issues such as anxiety and depressive symptoms. In turn, that can reduce the chances of long-term mental health ramifications.
Additionally, mental health professionals can offer strategies to help people navigate the social and educational hurdles that can be caused by illnesses.
This professional involvement and support can act as a strong buffer against more serious future mental health implications.
Wrapping Up
Early intervention and supportive environments can mitigate the potential long-term mental health effects of childhood illnesses.
So, if your child has an illness, make sure you take steps to lessen the impact that the illness could have on their mental health later in life. The first step is to contact a mental health professional.
Author Bio: Veronica Turner is a health and lifestyle writer with over 10 years of experience. She creates compelling content on nutrition, fitness, mental health, and overall wellness.”
Please also review AIHCP’s Health Care Life Coach Certificate program and see if it meets your academic and professional goals. These programs are online and independent study and open to qualified professionals seeking a four year certification.


 Written By Lucy Peters
Written By Lucy Peters