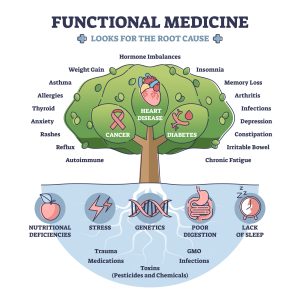
In the rapidly evolving landscape of modern healthcare, the demand for holistic nursing training has never been more critical. This approach, which emphasizes the interconnectedness of physical, mental, emotional, and spiritual wellbeing, offers a comprehensive form of patient care that transcends traditional medical practices. Holistic nursing melds the science of conventional medicine with the sensitivity of wellness coaching, making it an indispensable facet of contemporary healthcare. Its essence lies not only in treating the symptoms but in nurturing the whole person, equipping practitioners with the ability to deliver care that is both empathetic and scientifically sound.
Holistic nursing is a special way of caring for people. Instead of just looking at symptoms, holistic nurses see the whole person. They think about the mind, body, spirit, and environment. This kind of care helps people heal better and stay well. Holistic nurses use different methods and build strong relationships with their patients.
This article aims to unpack the essence and significance of holistic nursing training, outlining its core values, historical background, and the pivotal role it plays in modern healthcare systems. It will traverse the educational pathways and certifications necessary to become a certified holistic nurse, including holistic nursing programs and holistic nursing certification online. Furthermore, it will delve into the practical application of this discipline in various healthcare settings, highlighting career opportunities ranging from holistic nurse practitioners to integrative healing arts specialists. By providing a comprehensive overview, this discussion seeks to illuminate the transformative potential of holistic nursing in enhancing patient care and promoting the wellbeing of both caregivers and those they serve.
Key Takeaways
-
- Holistic nursing treats the whole person, not just symptoms.
- Holistic nurses use both traditional and alternative healing methods.
- Education for holistic nursing training includes degrees, certifications, and ongoing learning.
- Holistic nursing can be practiced in hospitals, private practices, and community settings.
- Holistic nurses create personalized care plans and empower their patients.
Understanding Holistic Nursing
Core Principles of Holistic Nursing
Holistic nursing is about caring for the whole person, not just their symptoms. This means looking at the body, mind, emotions, and spirit as one. Holistic nurses use their knowledge, skills, and intuition to help patients heal and feel whole. They work with patients to create a healing process that fits their unique needs and culture.
Defining Holistic Nursing
Holistic nursing is defined as a practice that aims to heal the whole person through the integration of all aspects of individual wellness. This includes physical, mental, emotional, spiritual, and environmental health. Holistic nurses strive to promote health by understanding the full spectrum of factors affecting patient well-being, and they treat the person, not just the symptoms.
The Role of the Holistic Nurse
A holistic nurse is more than just a caregiver; they are a partner in the patient’s healing journey. They build strong connections with their patients to understand their needs better. This helps them provide care that promotes overall well-being. Holistic nurses can work in any healthcare setting, from hospitals to private practices.
Holistic Nursing vs. Traditional Nursing
While traditional nursing often focuses on treating specific symptoms or illnesses, holistic nursing looks at the person as a whole. This approach allows for more personalized care plans that can lead to better outcomes. Holistic nurses believe that every patient is unique and deserves care that considers all aspects of their life.
The Philosophy Behind Holistic Nursing
The philosophy of holistic nursing is rooted in the understanding that an individual is not merely comprised of separate symptoms or issues but is a complex entity with interconnected dimensions. Holistic nursing recognizes two views on holism: one sees the person as a bio-psycho-social-spiritual whole where the whole is greater than the sum of its parts, and another views the individual as a unitary whole existing in mutual process with the environment . This philosophy guides nurses to appreciate the interconnectedness of the self with others, nature, and the spiritual, which is fundamental in fostering healing and wellness.
Scope and Practice
The scope of holistic nursing practice covers a wide array of patient care aspects, from traditional medical treatment to integrative approaches that include Complementary and Alternative Medicine (CAM). Holistic nurses utilize their knowledge, theories, expertise, intuition, and creativity to provide care that respects the patient’s health beliefs, values, and experiences. They are trained to use various CAM practices such as dietary advice, therapeutic massage, breathwork, and meditation alongside conventional medical treatments.
Holistic nursing is recognized by the American Nurses Association as a specialty with a defined scope and standards of practice. These standards ensure that holistic nurses meet the professional requirements to provide high-quality health care. The practice not only focuses on healing the physical body but also considers emotional and spiritual health, aiming to restore the patient’s overall harmony and balance.
The practice of holistic nursing requires a comprehensive educational background that includes both conventional healthcare training and specialized knowledge in holistic care practices. Holistic nurses are encouraged to pursue continuous learning to keep up with the evolving standards and practices in both general and holistic nursing fields.
By integrating both traditional and holistic approaches, holistic nurses play a crucial role in modern healthcare. They provide a more thorough understanding and care strategy that addresses all aspects of a patient’s life, promoting better health outcomes and a more satisfying patient experience.
The Core Values That Drive Holistic Nursing
Holistic nursing is anchored in a set of core values that guide the practice and ensure it remains focused on healing the whole person. These values encompass holistic philosophy and education, ethical principles, self-care for nurses, effective communication, and a caring process that is culturally competent and therapeutic.
Holistic Nursing Education
Education forms a cornerstone of holistic nursing, emphasizing a philosophy that integrates all aspects of human wellness. This educational approach encourages nurses to engage in continuous learning, reflection, and application of knowledge to enhance their practice and patient care. Holistic nursing education is not just about acquiring skills; it’s about embracing a broader understanding of health that includes physical, mental, emotional, spiritual, and environmental aspects.
The educational pathways for holistic nurses include foundational courses that explore the core values and prepare nurses for certification exams. These courses are essential for nurses aiming to deepen their practice in holistic care and achieve professional certification, which is supported by materials such as the “Holistic Nursing: Scope & Standards, 3rd Edition” and the “Holistic Nursing: A Handbook for Practice, 7th Edition” .
Holistic Ethics and Research Standards
Ethical practice is paramount in holistic nursing, guiding nurses to adhere to high standards of professional conduct and patient care. The core values of holistic nursing emphasize the importance of ethical principles such as autonomy, beneficence, nonmaleficence, veracity, confidentiality, justice, and fidelity. These principles ensure that holistic nurses provide care that respects patients’ health beliefs, values, and experiences, while also promoting safety and quality in nursing care.
Research also plays a critical role in informing holistic nursing practice. Nurses are encouraged to integrate evidence-based practices with patient preferences and clinical expertise to deliver optimal care. Competency in holistic nursing involves not only technical skills but also ethical care, cooperation with team members, leadership, and critical thinking. Holistic nurses continuously seek new knowledge and participate in research to keep their practice aligned with the latest standards and ethical guidelines provided by authoritative bodies such as the American Nurses Association and the American Holistic Nurses Association.
By adhering to these core values, holistic nurses enhance their ability to create therapeutic environments and engage in practices that honor the interconnectedness of body, mind, and spirit, ultimately leading to better health outcomes and a more satisfying patient experience.
Historical Overview of Holistic Nursing
Florence Nightingale’s philosophy profoundly influenced the foundation of holistic nursing. She believed that nursing should encompass care for the patient’s body, mind, and spirit, creating healing environments through the integration of heart, brain, and hands. Her environmental theory highlighted the necessity of clean water, air, basic sanitation, cleanliness, and light, emphasizing that a healthy environment is crucial for healing.
Nightingale advocated for a robust knowledge base in nursing, grounded in solid principles, to ensure quality care and critical decision-making in clinical practice. Her teachings stressed the importance of considering cultural and religious diversity, as well as the economic and social aspects that encompass care, thereby addressing the needs and concerns of individuals in their uniqueness.
The historical trajectory of Florence Nightingale showcases the critical role of nurses in thinking holistically and dealing with adversity, as evidenced during the Crimean War. Her legacy continues to influence modern holistic nursing, emphasizing the importance of a well-rounded approach to patient care.
Growth of Holistic Nursing in Modern Times
Since the 1700s, holistic principles have been embedded in nursing, incorporating natural remedies and healing therapies such as the use of medicinal herbs. However, by the mid-1900s, the focus shifted towards technology and profit, overshadowing the human connection fundamental to nursing. This shift led to the formation of the American Holistic Nurses Association (AHNA) in 1980, aimed at reviving holistic practices in nursing.
The AHNA established standards and a certification process to reinforce holistic practices among nurses. In 2000, the AHNA Standards of Holistic Nursing Practice were published, emphasizing the core values of holistic philosophy, ethics, education, and caring process, necessary for effective holistic nursing practice.
These standards were developed through extensive review and consensus-building among holistic nurses, reflecting a commitment to maintaining high standards in the practice. The American Holistic Nurses Certification Corporation (AHNCC), founded in 1997, further supports the professional development of holistic nurses, offering certifications that recognize advanced holistic nursing practices.
Today, holistic nursing continues to evolve, integrating modern medical practices with traditional holistic approaches, ensuring that the care provided addresses all aspects of a patient’s well-being. This integration supports better health outcomes and a more satisfying patient experience, demonstrating the enduring relevance of holistic nursing in contemporary healthcare.
Integrating Holistic Nursing in Modern Healthcare
Blending Traditional and Modern Practices
Holistic nursing care integrates both traditional and modern healthcare practices, focusing on treating the patient as a whole rather than just addressing specific symptoms. This blend is evident in settings like Taiwan, where healthcare systems combine traditional Chinese medicine (TCM) with Western medical practices. Patients have the option to choose between or integrate these modalities based on their personal beliefs and medical needs, which is a testament to a truly patient-centered approach.
Incorporating traditional practices such as dietary advice, herbal medicine, and acupuncture alongside conventional medical treatments allows for a comprehensive care strategy that addresses various aspects of a patient’s health. This approach not only enhances patient outcomes but also respects their cultural and personal preferences, thereby improving their overall satisfaction with the healthcare they receive.
Therapeutic Relationships
Holistic nurses build strong, healing relationships with their patients. These connections are based on trust and mutual respect. Nurses listen carefully to understand the needs and concerns of their patients, creating a safe space for healing.
Self-Care and Self-Reflection
Holistic nurses believe in taking care of themselves to better care for others. They practice self-reflection to understand their own feelings and thoughts. This helps them stay balanced and provide the best care possible.
Integrative Health Modalities
Holistic nursing training uses different methods to help patients heal. These can include traditional medicine, as well as alternative treatments like acupuncture or meditation. By combining these methods, they aim to treat the whole person, not just the illness.
Clinical Applications of Holistic Nursing
Holistic Nursing in Hospitals
Holistic nursing can be practiced in hospitals, where nurses focus on the whole person, not just the illness. They create caring environments that promote healing by considering the patient’s mind, body, and spirit. This approach helps patients feel more comfortable and supported during their hospital stay.
Private Practice Opportunities
In private practice, holistic nurses have the freedom to offer personalized care. They can spend more time with each patient, understanding their unique needs and preferences. This allows for a deeper connection and more effective healing process.
Community Health Settings
Holistic nursing training is also valuable in community health settings. Nurses work with diverse populations, addressing not only physical health but also emotional and social well-being. By focusing on the whole person, they help improve the overall health of the community.
Impact on Healthcare Systems
The integration of holistic nursing practices significantly impacts healthcare systems by improving the quality of care and patient safety. Studies have shown that holistic care can prevent diseases and death and enhance the quality of healthcare provided to patients. This is crucial in modern healthcare environments where the focus is increasingly on preventive care and the management of chronic conditions.
Holistic nursing practices are also associated with reduced hospitalization times and treatment costs. By addressing patients’ physical, emotional, social, and spiritual needs, holistic care restores their balances and enables them to better cope with their illnesses, consequently improving their lives. Furthermore, the practice of holistic care by nurses has been shown to have a major impact on patient outcomes, emphasizing the need for healthcare systems to support and enhance nurses’ ability to provide holistic care .
The challenges to integrating holistic nursing in healthcare systems often include a lack of resources, inadequate time, and the need for more comprehensive education and training in holistic practices. Overcoming these barriers requires a concerted effort from healthcare institutions to invest in holistic training programs and to foster an environment that supports the holistic model of care. This can be facilitated through policy changes, increased funding for holistic care initiatives, and a shift in healthcare culture to embrace and prioritize holistic health practices.
Educational Requirements and Pathways
Becoming a Holistic Nurse
To embark on a career as a holistic nurse, individuals must first meet the standard educational and holistic nursing training requirements necessary to become a registered nurse in their respective state. This typically involves completing either a two-year associate degree in nursing (ADN) or a four-year Bachelor of Science in Nursing (BSN). Given the increasing preference among employers for BSN-prepared nurses, many registered nurses (RNs) with an ADN opt to further their education through RN-to-BSN programs.
For those entering nursing from another field, accelerated BSN programs offer a pathway to become RNs in as little as 11-18 months, preparing them efficiently for a career in nursing . Upon completing their degree, aspiring holistic nurses must pass their state’s NCLEX-RN exam to obtain their RN license.
Certification and Continuing Education
In addition to certification, holistic nurses are encouraged to engage in continuous learning to adapt to evolving healthcare needs and maintain their licensure. This might include completing a certain number of Continuing Education Units (CEUs), which are essential for renewing an RN license. Holistic nurses may also explore certifications in complementary therapies such as massage therapy, acupuncture, and dietary coaching, each requiring its own specific holistic nursing training and certification.
Continuing Education Opportunities
Holistic nursing training helps one to enter a field that encourages lifelong learning. Continuing education opportunities allow you to stay updated on the latest holistic practices and research. These programs often include self-reflection, self-development, and self-care components, helping you grow both personally and professionally. By engaging in continuing education, you can enhance your expertise and provide better care to your patients.
Practical Application of Holistic Nursing
In the realm of holistic nursing, the practical application extends beyond conventional medical treatments to incorporate alternative and complementary therapies, which are integral in treating the patient as a whole. These therapies, often rooted in ancient traditions, are increasingly recognized for their efficacy and integration into modern healthcare practices.
Career Opportunities in Holistic Nursing
Employment Settings
Holistic nurses can find work in many places. They might work in hospitals, private practices, or even schools. Some also work in community health centers. Holistic nursing offers many job options.
Salary Expectations
The pay for holistic nurses can be different based on where they work and their experience. Some might earn more in private practice, while others might find good pay in hospitals. Overall, holistic nurses can expect a fair salary for their work.
Career Advancement
Holistic nurses have many ways to grow in their careers. They can take more classes to learn new skills or get special certificates. This helps them move up in their jobs and take on new roles. Holistic nursing is a field with many chances to advance.
Holistic Nursing and Patient Care
Personalized Care Plans
Holistic nurses see each patient as a unique individual, not just a list of symptoms. This approach helps them form meaningful connections and understand their patients’ needs better. By treating the whole person, they can create personalized care plans that promote healing and well-being.
Mind-Body Connection
Holistic nursing training helps us to consider the interconnectedness of a person’s body, mind, and spirit. This approach aims to create healing environments for both patients and healthcare providers. It recognizes that healthy relationships and a supportive environment are crucial for healing.
Patient Empowerment
Holistic nurses often educate patients and their families on healthy lifestyle practices and self-care techniques. This empowers patients to take an active role in their own healing process, making them partners in their own care.
Challenges and Rewards of Holistic Nursing
Common Challenges
Holistic nursing can be tough. Nurses often face skepticism from colleagues who prefer traditional methods. They also need to stay updated with both conventional and holistic practices, which can be time-consuming. Balancing these two approaches can be tricky and sometimes overwhelming.
Emotional and Professional Rewards
Despite the challenges, holistic nursing offers many rewards. Nurses form deep connections with their patients, understanding them as whole people, not just a set of symptoms. This meaningful bond can be very fulfilling. Additionally, holistic nurses often find personal growth through self-care and self-reflection, which are key parts of their training.
Balancing Traditional and Holistic Approaches
Finding the right balance between traditional and holistic methods is essential. Holistic nurses must integrate both approaches to provide the best care. This balance allows them to offer personalized care plans that promote overall well-being. While it can be challenging, the ability to blend these methods effectively is a significant reward in itself.
Alternative and Complementary Therapies
Holistic nursing leverages a variety of alternative and complementary therapies (CAM), which include practices such as Ayurveda, homeopathy, naturopathy, and traditional Chinese medicine. These systems are characterized by their holistic approach to health, emphasizing the patient’s entire well-being rather than focusing solely on symptom management. For instance, Ayurveda, with its origins over 5,000 years ago in India, involves treatments like yoga, meditation, and dietary modifications tailored to individual needs.
The use of CAM therapies is not static; it evolves as certain practices gain empirical support and become integrated into mainstream healthcare. This dynamic nature of CAM allows it to complement traditional Western medicine, often leading to what is known as integrative medicine—where both conventional and alternative methods are used to stimulate the body’s natural healing response.
Patient Case Studies
The effectiveness of holistic nursing can further be illustrated through patient case studies. For example, Ms. Linda Mogen, a 76-year-old retired school teacher with a history of diabetes, hypertension, and other health issues, exemplifies the successful integration of holistic care in managing chronic conditions . Ms. Mogen’s treatment plan includes regular medical check-ups and insulin therapy complemented by alternative medicine like Barley Green Herb and other supplements. Her holistic care extends beyond physical treatment to encompass emotional and spiritual well-being, supported by her strong social connections and personal education about her conditions.
Ms. Mogen’s case is a testament to the holistic nursing approach that considers not just the biological aspects of health but also the psychological, spiritual, and social dimensions. Her care strategy, influenced by her background and beliefs, highlights the personalized nature of holistic nursing, which tailors care plans to the unique needs and life circumstances of each patient.
The practical application of holistic nursing, through both alternative therapies and personalized patient care, demonstrates its critical role in contemporary healthcare. By addressing the comprehensive needs of patients, holistic nursing not only improves health outcomes but also enhances the quality of life, making it a vital component of modern medical practice.
Career Opportunities and Professional Growth
Work Environments for Holistic Nurses
Holistic nurses find employment in a diverse array of settings, reflecting the versatile nature of their training and skills. A significant proportion of holistic nurses work in acute care hospitals, where they constitute about 35% of the workforce in this specialty. Additionally, universities and colleges employ around 20% of holistic nurses, providing opportunities for these professionals to contribute to education and research in health sciences. Private practices also account for another 20% of employment, offering a more personalized approach to patient care.
Other notable areas where holistic nurses practice include home healthcare, hospice, palliative care, long-term care facilities, and consultancies. These environments allow holistic nurses to apply their skills in non-traditional settings, enhancing the scope of holistic care. The flexibility of holistic nursing is further demonstrated in specialized settings such as birth centers and academic or educational institutions, where they play crucial roles in teaching and guiding future generations of healthcare professionals.
Salaries and Job Outlook
The financial aspect of a career in holistic nursing can be quite rewarding, albeit influenced by various factors such as the nurse’s level of education, years of experience, and geographical location of employment. On average, holistic nurses earn an annual salary of $85,779, with potential earnings ranging from $21,500 to $137,000 depending on the aforementioned variables.
States like California, Washington, and Wyoming offer the highest salaries, reflecting the high demand and cost of living in these regions. For instance, cities such as Santa Clara and San Francisco in California report average salaries of $105,712 and $102,045, respectively. This variation underscores the significant impact of location on earning potential in the field of holistic nursing.
The job outlook for holistic nurses is also positive, with an anticipated increase in employment opportunities. The Bureau of Labor Statistics projects a 6% growth in the employment of registered nurses from 2021 to 2031, which is expected to include holistic nurses as the demand for preventative and integrative care continues to rise . This growth is supported by an increasing public interest in complementary and alternative medicine, ensuring a steady demand for skilled holistic nurses.
In conclusion, holistic nursing offers a range of career opportunities across various healthcare settings, accompanied by competitive salaries and a positive job outlook. These factors make it an appealing and viable career path for individuals interested in a nursing career that embraces a comprehensive approach to health and wellness.
Conclusion
The journey through the realms of holistic nursing underscores its indispensable role in modern healthcare, providing a nuanced understanding of patient care that recognizes and treats the interconnectedness of the physical, mental, emotional, and spiritual dimensions of health. This comprehensive approach, stemming from a rich historical foundation and encapsulated within a rigorous educational and practical framework, offers a transformative potential for enhancing patient care and outcomes. By embracing both traditional and innovative practices, holistic nursing serves as a beacon for a more empathetic, effective, and integrated healthcare system.
As we look toward the future of healthcare, the principles and practices of holistic nursing stand out as essential components in addressing the complex needs of patients in a more holistic, compassionate, and personalized manner. The significance of this field cannot be overstated, with its implications for improved health outcomes, patient satisfaction, and the overall wellbeing of both caregivers and those they serve. Encouraging the integration and appreciation of holistic nursing within the healthcare landscape reaffirms our commitment to a more inclusive, understanding, and human-centered approach to healthcare.
Do you want to take some Holistic Nursing Training? We offer an online Holistic Healthcare certification program. Our 6 online Holistic Nursing training courses will prepare you to enter the field of holistic and integrative healthcare! Our program starts with the basic framework of holistic nursing and then moves onto advanced holistic concepts and integrative methods. For more information please visit our site here.
FAQs
- What is holistic nursing?
Holistic nursing is a type of nursing that cares for the whole person. This means looking at the body, mind, emotions, spirit, and environment together, not just treating symptoms. - How do holistic nurses differ from traditional nurses?
Holistic nurses focus on the entire well-being of a patient, including mental and emotional health, while traditional nurses often focus mainly on physical health. - What education is required to become a holistic nurse?
To become a holistic nurse, you need a nursing degree and a registered nurse (RN) license. Additional training in holistic health practices like meditation and acupuncture is also helpful. - Where can holistic nurses work?
Holistic nurses can work in many places, including hospitals, private practices, community health centers, and schools. - What are some common holistic nursing practices?
Some common practices include massage, meditation, aromatherapy, and wellness coaching. - Is holistic nursing recognized by professional organizations?
Yes, holistic nursing is recognized by professional organizations such as the American Holistic Nursing Association (AHNA). - What makes holistic care crucial in the nursing field?
Holistic nursing is vital in healthcare as it embraces the complete interconnectedness of an individual’s physical, emotional, spiritual, and social health. This method of nursing focuses on treating the entire person, not just the symptoms or diseases they may be experiencing. - What is driving the rise in popularity of holistic nursing?
The increasing popularity of holistic nursing can be attributed to a shift towards a more comprehensive understanding of well-being, which stresses the importance of the unity of mind, body, and spirit in achieving optimal health. - What is the significance of holistic healthcare?
Holistic healthcare is crucial as it promotes the recognition of the entire individual, encompassing physical, mental, emotional, social, intellectual, and spiritual aspects. It actively involves individuals in their health decisions and healing processes, fostering wellness-oriented lifestyle choices. - Why is holistic nursing particularly important in end-of-life care?
Holistic nursing plays a critical role in end-of-life care by focusing on treating a patient’s comprehensive needs when curing the disease is no longer feasible. This approach facilitates discussions about death, fulfills last wishes, and eases the grieving process for both patients and their families.
Research Articles:
Holistic nursing care practice and associated factors among nurses in public hospitals of Wolaita zone, South Ethiopia. Ambushe, S.A., Awoke, N., Demissie, B.W. et al. BMC Nurs 22, 390 (2023).
Access link here
The relationship between the ethical attitudes and holistic competence levels of intensive care nurses: A cross-sectional study. Nihal Taşkıran ,Gulengun Turk PLOS One Published: July 13, 2023
Access link here
Building Spiritual Care Competency in Undergraduate Psychiatric Mental Health Nursing Students: A Quality Improvement Project. Bush RS, Baliko B, Raynor P. Journal of Holistic Nursing. 2023;41(3):256-264.
Access link here
Integrating Implicit Bias Training for Undergraduate Holistic Admission Reviewers. Angela D. Alston, DNP, MPH, APRN-CNP, WHNP-BC, FNP-BC, FNAP and Amy Jauch, DNP, RN, CNE. Journal of Nursing Education, 2024;0(0):1–4. Published Online: June 21, 2024
Access link here